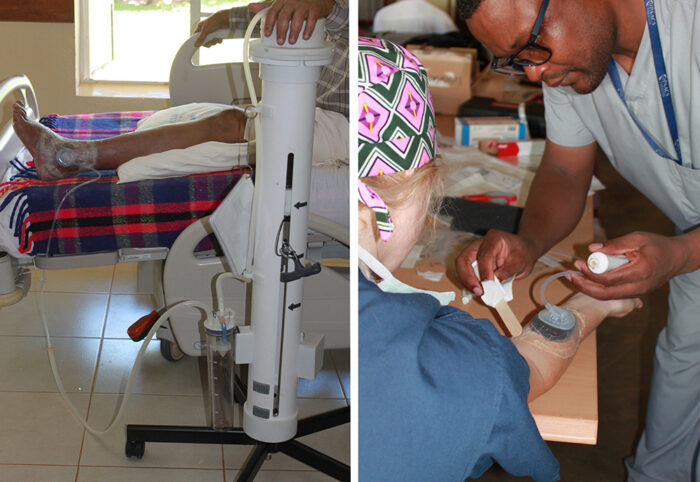
KupolaCare Paves the Way for Improved Wound Care
Members of the Design Outreach team just returned from Malawi and Kenya where they met with clinicians at Malamulo Mission Hospital and Kapsowar Mission Hospital to implement and observe recent updates to the KupolaCare™ wound dressing material and application technique. They also set out to learn more about procurement and purchasing for mission hospitals to determine a plan for scaling the project to more medical facilities across Africa.
We caught up with Medical Engineering Team Lead Hannah Tilley and Project Engineer Ellie Rider to hear more about their trip and were moved by their stories of hope and healing. We hope this snapshot of our conversation with them is as inspiring to you as it was to us!
What were you hoping to accomplish during this trip, and what were the expected outcomes?
Ellie: We were hoping to fully train clinicians on the new dressing seal technique and observe them using it. We were cautiously expecting this seal technique to allow our device to be more easily used and used for larger wounds as well and were incredibly happy with the results. We also were hoping to observe lots of wound care—both with and without Negative Pressure Wound Therapy (NPWT). Finally, we wanted to gain some insight into how the hospitals are receiving both smaller consumables and larger devices. This highlighted some possible partners for us as we look into providing KupolaCare.
What excites you most about launching KupolaCare in these hospitals?
Ellie: It’s incredible to be here and meet the people who need this therapy. Malamulo hospital previously had no way to administer NPWT. When they can’t heal wounds on extremities, amputation is the next best option, but it is crippling for someone’s livelihood. I’m so excited to be able to give these patients a great chance for healing where before it was much slimmer. Kapsowar Hospital in Kenya has become a wound care center, receiving difficult wounds from all over the country. This is because Dr. Celeste Adrian and her husband have rigged suction machines to work as NPWT devices. As we are here, Dr. Adrian has 28 wound care patients. She has 7 suction devices that all rely on unreliable electricity. Recently, the power went out in the night and the generator wasn’t working either. This left the patients treated with the suction devices without therapy for over an hour, which is dangerous for these wounds as it can cause infection. The KupolaCare device does not require electricity and is unaffected by power outages. Bringing KupolaCare here means that more of these patients who travel long and far for healing will be able to receive this life changing therapy—and in a more reliable way.
How do you think KupolaCare will help staff care for patients differently than before?
Hannah: When compared with other wound care practices, KupolaCare provides an improvement in care, cost savings, and sustainable treatment option for hospitals and patients. A common treatment for wounds is the standard wet-to-dry dressing change. This is typically performed daily. It can become expensive for patients to purchase materials every day. It is also a painful process to remove bandages and clean the wound daily. KupolaCare dressings follow typical NPWT practices, and dressings are changed every 3 days. This omits a daily cost and hassle or pain of removing a dressing every day. This type of advanced wound care has also proven to be very effective at closing the wound and bringing blood flow, nutrients, and healing to the wound bed as compared with standard wet to dry dressing changes. The devices also do not rely on electricity, allowing them to continuously provide therapy. Patients and healthcare providers can rest knowing the devices continue working during the frequent power outages and walks to the restroom or outdoors.
What have you learned from training hospital staff so far?
Hannah: Interactions with the hospital staff and the setting this device will be used in are important to the development and design of the device. Since we are not healthcare providers, it is very helpful to hear the perspectives of the hospital staff. During our time with them, they provide valuable comments and feedback about the device. One example of a learning from this past trip was getting feedback on how the tubings are connected to the exudate container lid. Even after training, there was one tubing connection that was a bit unclear. This tells us that we need to design this in a way that is more intuitive and user-friendly. We need to design out any potential for misconnections.
How does your work with KupolaCare at these hospitals help DO’s long-term mission of providing sustainable medical technology?
Ellie: Our work with Malamulo and Kapsowar is the culmination of years of hard work. Seeing everything falling into place with our device finally healing patients is a huge blessing. The hospitals that we’re working with have told us that they chronically don’t have enough resources. It’s a struggle to afford certain materials, but it’s also a struggle to even find out how to source them. On a hospital tour in Kenya, we were shown their storage rooms, which were filled top to bottom with broken medical equipment. Some had notes taped onto them with scribbles about which components were broken or what parts they would need. An engineer at that hospital told us that they keep it all in case they get a tool or part donated that could fix it. It’s difficult to see the patients at the hospital hopeful for healing and at the same time know how difficult it is for the hospital to find what they need to bring healing. Watching the KupolaCare device in use gives me hope that through this work we can alleviate some of this strife by providing devices specifically for use in their context.
What has been most impactful about working on this project?
Ellie: It has been so impactful to be able to meet patients who are awaiting treatment for their wounds. More than just the physical healing, it is so impactful to bring this healing in the name of Jesus. To be able to sit with patients and pray for them has been incredible. The best part of this work is that it’s not our own. It’s all in the hands of the Lord.
–––––––
During the trip, Hannah and Ellie had a chance to talk with Dr. Brent Sherwin from Malamulo and Dr. Celeste Adrian from Kapsowar, who emphasized the great need for a device like KupolaCare that can provide reliable wound treatment even in remote and under-resourced settings. One of the questions the team asked is “What message do you want to share with the people who made this project possible?” This is what they said:
Dr. Sherwin:
“There are a lot of projects you can get involved with and a lot of NGOs you can donate to. But one of the things I appreciate about Design Outreach is that they’re very transparent about what they’re trying to do—and about the results they’re getting. That’s one of the things that I really appreciate about this device—it’s being done properly. It’s not just something that kind of works not so great and we stop using it. The team keeps coming back. It’s continual process improvement. So for the donors, a big thank you for putting their energies into this device. But I think it is important for donors to know that the team on the ground is also putting a lot of effort in to use their money, to go as far as they can, and to come up with a good product. When the project’s completed, I think it will have a huge impact not only in our hospital but, ideally, across the continent. It’s the most sustainable wound vac I’ve ever seen as far as being able to get the parts, reproduce them, the durability, and reusability—those are all very important things that we value as a low-resource facility, and that is what the donors are allowing DO to do with the funds.”
Dr. Adrian:
“A lot of my patients that have had wounds for 20 to 40 years—actually, 55 was my record—bounced around from hospital to hospital. Generally, nobody really takes them on; they just get the wound cleaned every couple of days for decades. But nobody really has the means to actually get them healed. And then people with really bad wounds wind up in hospice just waiting to die. So when we started using NPWT here and started saying, “No, this can be treated,” word just started spreading. Just today, I got another hospice referral from somebody whose wounds were deemed bad enough that he should just be allowed to pass, but that hospital is aware of the work we’re doing and so they’ve sent him our way. Word of mouth is incredibly powerful in Kenya, so we’re now getting patients from everywhere.
Obviously, we’re very appreciative of every effort to make [this device] something that I can use, but also something that we may be able to get into hospitals all over the place and be able to provide wound care in many centers. And once we get through the learning phase and can get them out to other hospitals, this is potentially really going to change wound care.”